A metacarpal fracture is a type of bone fracture (broken bone). Your metacarpals are the bones in your hand that connect your thumb and finger bones (your phalanges) to your wrist. You can feel your metacarpals by pressing on the back of your hand.
Metacarpal fractures are one of the most common orthopedic injuries, caused by direct trauma like falls or punches, often seen in contact sports or from hitting hard surfaces. The most well-known type of metacarpal fractures is the “boxer’s fracture”.
A boxer’s fracture is a common break of the fifth metacarpal bone in the hand, occurring when someone punches a hard object with a closed fist or falls on his hand, causing the “neck” of the bone—the weakest point near the little finger—to fracture. Symptoms include pain, swelling, bruising, a visible deformity where the little finger meets the hand, and a limited ability to close the fist. Diagnosis is made through a physical exam and X-ray, and treatment typically involves a cast or splint, though severe cases may require surgery.
The most common type of metacarpal fracture is a boxer’s fracture, which is a break in the neck of the 5th metacarpal bone, often from punching a hard object. Fractures of the 1st (thumb) metacarpal bone, particularly at the base, are also very common and can happen from falls or direct trauma. Metacarpal fractures are common injuries in adolescents and young adults, particularly in the 5th (pinky) and 1st (thumb) metacarpal bones, often resulting from punching rocks or other direct impacts.
The metacarpals are the five bones in your palm that connect the wrist to the fingers. Each metacarpal has a base, shaft, and head, with the heads forming the knuckles where the bones connect to the finger bones (phalanges).
Metacarpal fractures can affect the bone’s shaft or head, with shaft fractures being more common, while base fractures are rarer and typically less impactful due to limited movement at that joint.
If a metacarpal fracture is displaced (out of alignment) or unstable, it can lead to functional problems and significantly impair hand and finger movement.
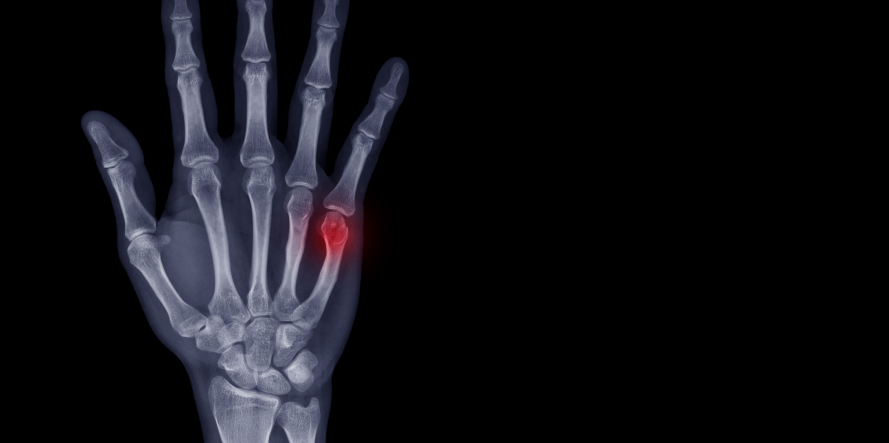
The location of your metacarpal fracture may impact where you feel symptoms. The main symptoms of a metacarpal fracture include:
Pain caused by a metacarpal fracture often worsens when you move, grip, or squeeze with your hand. This pain is usually the most severe in the first few days after the fracture happens.
A metacarpal fracture is diagnosed by an X-ray but requires a complete medical history, especially focusing on the injury’s cause and prior hand surgeries, and a physical exam to detect rotational deformities not visible on X-rays. The treatment plan hinges on the fracture’s location, displacement, rotational deformity, and soft tissue condition.
Diagnosis Process
A thorough history is taken to understand the mechanism of injury, the timeframe, any associated events, and prior hand or upper limb surgeries. Information about the patient’s occupation and athletic activities is also relevant.
Visual Inspection: Look for signs of swelling, bruising, and skin lacerations that could indicate an open fracture.
Rotational Deformity: A key part of the exam involves assessing finger malalignment. You can check for “scissoring” or overlapping of the fingers when the patient makes a loose fist.
Neurovascular Status: Assess for nerve damage and blood flow to the hand by checking capillary refill and two-point discrimination.
An X-ray is crucial to confirm the fracture, determine the location, and assess the extent of displacement. A CT scan may provide more detailed, three-dimensional images for complex injuries or to aid pre-operative planning.
Then, a treatment plan follows that is based on various factors, such as the location and type of fracture, the degree of displacement and rotational deformity, as well as the condition of the surrounding soft tissues.
Non-displaced or minimally displaced metacarpal fractures at the base and shaft, especially those without rotational deformity, are typically treated conservatively with a splint for 3-4 weeks to promote healing in the correct position. This immobilization helps prevent the fracture fragments from moving out of place, but may be followed by physiotherapy to restore hand function and prevent stiffness.
Physiotherapy is crucial for metacarpal fracture rehabilitation, focusing on gradual mobilization to prevent stiffness and restore hand function, which typically takes about 6 weeks for unrestricted use, though avoiding heavy lifting and contact sports is recommended until 8 weeks. Treatment involves exercises like “tendon glides” and, later, strengthening with putty, alongside potential scar management and swelling control. The overall prognosis for metacarpal fractures is generally good with appropriate management, though the specific treatment and timeline depend on the fracture’s type and any complications.
Conservative (non-surgical) treatment is suitable only for specific, stable finger fractures with minimal displacement, while surgery is indicated for non-reducible, open, multiple, or unstable fractures with significant shortening or rotational deformity. The recommended surgical procedure is closed or open reduction and osteosynthesis with plates, screws or a combination of both to ensure stability and functional recovery.
Dr. Panagiotis Pantos is a specialist Upper Limb Orthopedic Surgeon who has remarkable experience in osteosynthesis surgeries, even for the most comminuted fractures, achieving excellent functional outcomes.
Fill in your details below and we will contact you immediately!
WIN THE
MATCH POINT IN THE RACE
OF YOUR HEALTH!